
Strengthening the immune system with Vitamin D in light of COVID-19
In the last two decades, research has shown that our innate immunity and the modulation of our immune system is regulated in part through vitamin D (Grant, et al). Scientists from Spain outlined the multiple ways that Vitamin D interfaces with our respiratory system. They explain that when vitamin D interacts with its receptors in the immune system, it: (1) decreases the cytokine storm (2) regulates the activity of white blood cells (3) helps to maintain and (4) repair the cell walls within the air sacs of our lungs and finally it mitigates against abnormal clotting (Quesada-Gomez, MJ, et al). They illustrate these mechanisms in this graphic:

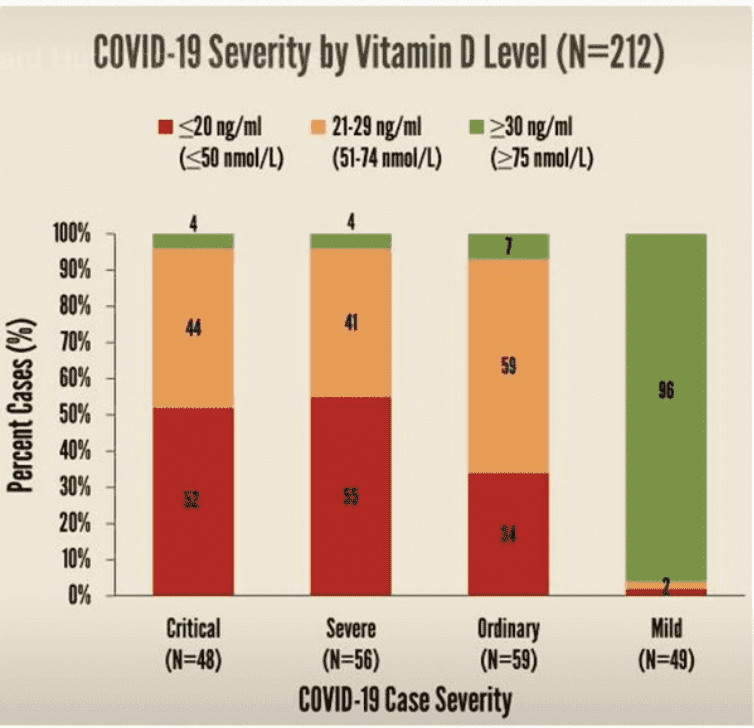
As an example of the impact of Vitamin D on the immune system we can look at some data from COVID-19 recovery. Data analyzed from 780 COVID patients in Indonesia, show that those patients who had low vitamin D levels, had worse courses of COVID illness than those with normal or high levels of D. The risk of death was ten times higher for those with severe vitamin D deficiency (less <20ng/ml) than for those with normal to high levels (Rahasuhan, P. et al). When we recognize, for example, that blood pressure control reduces all cause mortality by a factor of 1.5 (Kuriakose), we can appreciate even more how an opportunity to reduce COVID related mortality by a factor of 10 is very significant.

Data sourced from Rahasurun, Table 4.
Graph attributed--Ivor Cummins.
Vitamin D insufficiency is a widespread problem. Among caucasian Americans, the numbers of people with vitamin D levels under 30 ng/ml increased from 50% to over 70% from 1988 to 2004. In the Hispanic community 90% of its members are deficient with levels less than 30 ng/ml and in the African American community the incidence of vitamin D deficiency is 97% (McCullough, et al). Eighty percent of vitamin D is obtained through the skin. The melanin in darker skin prevents the manufacturing of vitamin D.
A great deal of human heartache could be avoided in the African American community if the necessity of raising vitamin D3 levels became common knowledge. Cancer and autoimmune disorders could be prevented and maternal and neonatal health could be improved.
What dose of Vitamin D should I take?
If you don’t know your vitamin D level, a blood sample can be drawn in our office very inexpensively. Although lab results are reported as normal if levels are above 30 ng/ml, the actual level needed to achieve bone health is 32 ng/ml.
During the last five years, many studies regarding vitamin D were funded, most likely due to an increase in research funding related to COVID19. Many studies confirmed what we observed in practice; that keeping vit D levels between 50 -80 ng/ml strengthens human immune health. Doses of 10,000 IU a day can be considered safe, as we know that 30 minutes of exposure to sunlight on the skin produces 10,000-25,000 IU of vitamin D. This is the upper tolerable daily limit for adults as set by the Endocrine Society. It is important to take vitamin D daily, as opposed to weekly, because vitamin D3 has a short half life within the body. Doses higher than 10,000 IU a day might be necessary for people who are obese or who have other clinical conditions like diabetes or chronic kidney disease. Doses higher than 10,000 IU/day require medical supervision.
Why are there different recommended doses?
There is controversy within the medical community about the correct dosing of vitamin D. For example, the Institute of Medicine’s Recommended Daily Allowance (RDA) for vitamin D is much lower than stated here. The Endocrine Society advocates much higher doses (McCullough, et al). Patrick McCoullough, MD has recently published the paper “Biosynthesis of Endogenous Antimicrobial Peptides May Explain Why Deficiency Increases Mortality Risk in COVID-19 Infections”, and also advocates for maintenance vitamin D doses of 10,000 IU for adults. In his paper he notes that vitamin D helps produce substances called antimicrobial peptides in immune cells that assist in fighting infections. These antimicrobial peptides have the ability to disrupt bacterial membranes and viral envelopes.
These anti-microbial peptides were important for fighting infections. Dr. McCullough stated: “The fact that 71.9% of NH (non-Hispanic) blacks are estimated to have serum 25(OH)D concentrations < 20 ng/ml, while 29% were < 10ng/ml in the 2009 report is a call for action, as these serum 25(OH)D concentrations are unable to effectively sustain production of antimicrobial peptides in response to infections, and could provide one explanation for why COVID-19 is killing NH blacks at an alarming rate and has been twice as deadly for both NH blacks and Latinos as compared to whites in New York City” p. 13.
What kind of vitamin D should I take?
You need to take vitamin D3, not D2. See your pharmacist to select a brand of vitamin D3. The least expensive source to obtain vitamin D is through being in the sun. Sunscreens and glass will block the UVB rays, and so sunshine is not a possibility for everyone. Again to be clear: African Americans are not able to absorb the necessary amount of UVB rays in the northern hemisphere in adequate amounts to create vitamin D3 in their bodies and usually must rely on supplementation.
Do I have to be concerned about calcium toxicity at 10,000 IU/day?
Dr. McCoullough’s team has tracked patients taking 5000-10000 IU/day, within an inpatient setting. They carefully monitored patients’ calcium levels among several thousand patients under their protocol, none had an incident of hypercalcemia. Their study, along with others gives indication that vitamin D doses of this level ought to be safe. (Billington, et al) (Jetty, et al) Anyone with compromised kidneys ought to have their calcium levels can be tracked by your physician while taking higher doses of vitamin D.
What about doses for children?
The Endocrine Society recommends 400-600 IU daily for infants 0-11 months and 600-1000 IU daily for children ages 1 through 18 years of age, for maintenance doses. McCullough discusses that when deficiency is present, the Endocrine Society has published higher upper tolerable daily intake limits. The upper tolerable daily intake limits are 2000 IU for infants 0-11, and 4000 IU for children ages 1 through 18 years of age. Overweight children will need a greater dose adjusted by their physicians. Breast fed infants do receive vitamin D from their mothers via breast milk in sufficient quantities without supplementation, if mothers are taking 6000 IU per day. Maternal supplementation is essential. (Hollis, et al) (Jain, et al). Non-breast fed infants require vitamin D supplementation.
If I have not been taking Vitamin D and begin to take physiological doses now, will that give me the protection that I need immediately?
No, it will not. There are different ‘loading dose’ schedules that have been suggested in the medical literature. I would encourage you to call our office if you need help sorting out that question.
Is there anything else that I need in addition to Vitamin D, in order for it to be effective?
Yes, magnesium is necessary for vitamin D to be effective within the body. It is estimated that 75% of Americans are magnesium deficient. While many foods ought to contain magnesium, the mineral depletion of soil and highly processed foods have contributed to magnesium deficiency. The Recommended Daily Allowance (RDA) for magnesium is 320mg for women and 400mg for men.
In order for your body to create the biologically active form of vitamin D, magnesium must be present, because it serves as a cofactor in the vitamin D converting enzymes. There are many types of oral magnesium supplements. Dr. Carolyn Dean has done extensive research on magnesium and her resources are available here at drcarolyndean.com.
If this is so important, then why is this information not more widely discussed?
We do not have an answer to that question. However, thirty clinicians and researchers signed a letter to the editor of the British Medical Journal commenting on the irony of the slowness of society to apply this strategy:
“Human nature is such that simple solutions to complex issues, for example vitamin C for scurvy, and hand washing prior to baby delivery, are often not readily embraced; but surely the scale and impact of the COVID-19 pandemic demands all avenues are fully explored; more so when no other effective treatment strategies as yet exist. A safe simple step, the correction of a deficiency state, vitamin D this time, convincingly holds out a potential, significant, feasible ‘COVID-19 mitigation remedy. (Brown, et al.)”
The data gathered in the last five years vindicates the 'vitamin D takers' and ought to encourage everyone else to get their D level checked and ensure this important nutrient is circulating in their body.
Billington, EO, et al. “Safety of High-Dose Vitamin D Supplementation: Secondary Analysis of a Randomized Controlled Trial.” The Journal of Clinical Endocrinology & Metabolism, 2019, doi:10.1210/clinem/dgz212.
Brown, RA and Rhein, HM. “Rapid Response: Is Ethnicity Linked to Incidence or Outcomes of Covid-19? .” BMJ, 24 Apr. 202AD, www.bmj.com/content/369/bmj.m1548/rr-6. Accessed June 3, 2020
Butterfield, S. “Experts debate pros, cons of vitamin D”. ACP Internist, November/December, 2009. https://acpinternist.org/archives/2009/11/vitamin.htm Accessed June 18, 2020.
Cummins, I. Ep. 73 Vitamin D Status and Viral Interactions…The Science https://www.youtube.com/watch?v=aXw3XqwSZFo&t=129s
Ebadi, M., Montano-Loza, A.J. Perspective: improving vitamin D status in the management of COVID-19. Eur J Clin Nutr (2020). https://doi.org/10.1038/s41430-020-0661-0 as accessed in nature.com June 3, 2020 https://www.nature.com/articles/s41430-020-0661-0#citeas
Grant WB, Lahore H, McDonnell SL, et al. Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths. Nutrients. 2020;12(4):988. Published 2020 Apr 2. doi:10.3390/nu12040988. Accessed June 3, 2020. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7231123/
Heaney RP, Davies KM, Chen TC, Holick MF, Barger-Lux MJ. “Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol” [published correction appears in Am J Clin Nutr. 2003 Nov;78(5):1047]. Am J Clin Nutr. 2003;77(1):204‐210. doi:10.1093/ajcn/77.1.204 accessed June 3, 2020. https://pubmed.ncbi.nlm.nih.gov/12499343/
Hollis, B.W., Wagner, C.L., Howard, CR,, Ebeling, HM., Shary, JR., Smith, PG , Taylor, SN., Morella, K., Lawrence, RA, Hulsey, TC, “Maternal Versus Infant Vitamin D Supplementation During Lactation: A Randomized Controlled Trial”. Pediatrics October 2015, 136 (4) 625-634 https://doi.org/10.1542/peds.2015-1669 accessed June 3, 2020
Jain, V. et al. “Vitamin D deficiency in healthy breastfed term infants at 3 months & their mothers in India: seasonal variation & determinants.” The Indian journal of medical research vol. 133,3 (2011): 267-73.
Jetty, V. et al. “Safety of 50,000-100,000 Units of Vitamin D3/Week in Vitamin D-Deficient, Hypercholesterolemic Patients with Reversible Statin Intolerance.” North American Journal of Medical Sciences vol. 8,3 (2016): 156-62. doi:10.4103/1947-2714.179133
Khazai, N. et al. “Calcium and vitamin D: skeletal and extraskeletal health.” Current rheumatology reports vol. 10,2 (2008): 110-7. doi:10.1007/s11926-008-0020-y
Kuriakose, A. et al. “Rate and Risk of All Cause Mortality among People with Known Hypertension in a Rural Community of Southern Kerala, India: The Results from the Prolife Cohort.” International journal of preventive medicine vol. 5,5 (2014): 596-603. Accessed June 3, 2020. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4050680/#:~:text=Among%20the%20people%20with%20high,those%20with%20a%20normal%20BP.
Quesada-Gomez, MJ, Castillo, ME. Vitamin D Receptor stimulation to reduce Acute Respiratory Distress Syndrome (ARDS) in patients with Coronavirus SARS-CoV-2 infections. The Journal of Steroid Biochemistry and Molecular Biology. Preprint June 11, 2020. Accessed June 19, 2020.
Meltzer, D., et al. Association of Vitamin D Deficiency and Treatment with COVID-19 Incidence, https://www.medrxiv.org/content/10.1101/2020.05.08.20095893v1
McCullough, PJ.; Amend, J.; McCullough, WP; Repas, SJ.; Travers, JB; Lehrer, DS,. The Essential Role of Vitamin D in the “Biosynthesis of Endogenous Antimicrobial Peptides May Explain Why Deficiency Increases Mortality Risk in COVID-19 Infections”. Preprints 2020, 2020050265 (doi: 10.20944/preprints202005.0265.v1).https://www.preprints.org/manuscript/202005.0265/v1
Mazzoleni S, Magni G, Toderini D. Effect of vitamin D3 seasonal supplementation with 1500 IU/day in north Italian children (DINOS study). Ital J Pediatr. 2019;45(1):18. Published 2019 Jan 28. doi:10.1186/s13052-018-0590-x
Quesada-Gomez, MJ, Castillo, ME. Vitamin D Receptor stimulation to reduce Acute Respiratory Distress Syndrome (ARDS) in patients with Coronavirus SARS-CoV-2 infections. The Journal of Steroid Biochemistry and Molecular Biology. Preprint June 11, 2020. Accessed June 19, 2020. https://www.sciencedirect.com/science/article/pii/S0960076020302442#!
Raharusun, P.; Priambada, S. ; Budiarti, C.; Agung, E.; Budi, C. Patterns of COVID-19 Mortality and Vitamin D: An Indonesian Study (April 26, 2020). Available at SSRN: https://ssrn.com/abstract=3585561 or http://dx.doi.org/10.2139/ssrn.3585561. Note: Dr. Raharusun organized this study with his own efforts, without any outside funding. He has subsequently passed away, not from COVID. We note our thanks to him and honor his memory.
Uwitonze, A. M., Razzaque, M.S., “Role of Magnesium in Vitamin D Activation and Function”. The Journal of the American Osteopathic Association, March 2018. Accessed June 3, 2020. https://docs.google.com/document/d/1G3QtmvP2MGBrplOTMv7jFvQt8WccfSYtJA0qw9elGFo/edit#
You Might Also Enjoy...


STAVING OFF ALZHEIMER’S — MORE REASONS TO ADOPT HEALTHY HABITS


